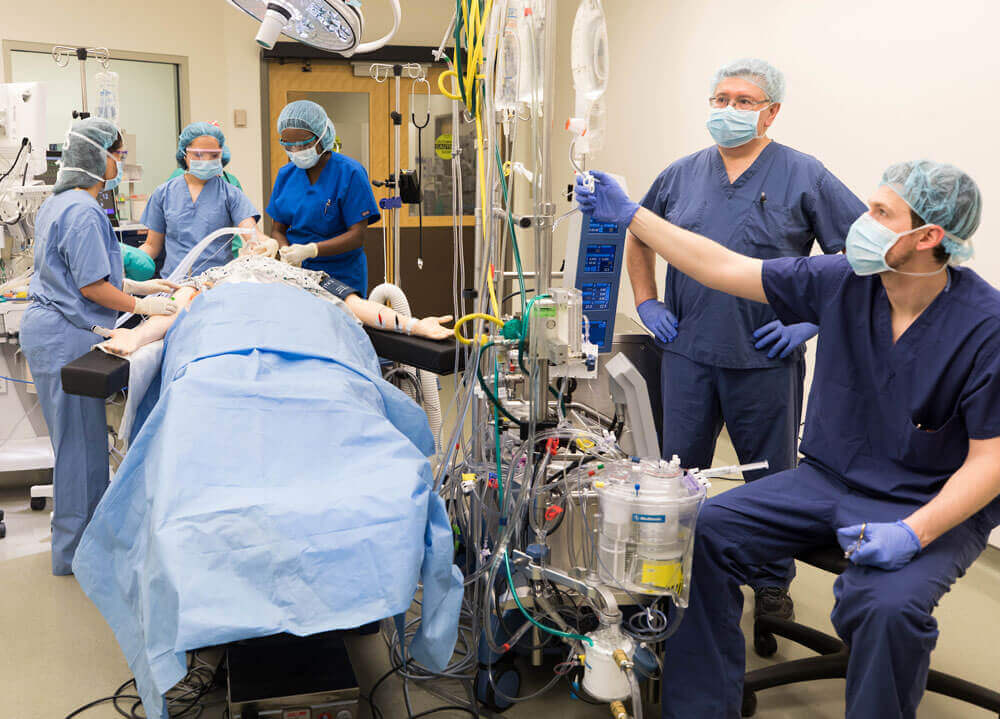
Cardiac operation in patients with sickle cell disease is a challenge to the surgical team. Performing cardiac surgery with the use of cardiopulmonary bypass (CPB) on patients with sickle cell disease requires extensive preoperative preparations and coordination from hematology, cardiac surgery, anesthetist, perfusion team and blood bank. CPB is commonly associated with hypothermia, hypoxia, hypoperfusion, and acidosis, which are pre-disposing factors that can trigger sickle cell crisis. Thus, careful attention to detail is vital to achieve the successful completion of the procedure safely, without triggering fatal vaso-occlusive episodes.
Here we describe our successful management of three sickle cell patients who underwent: 1) Aortic valve replacement with mitral valve repair 2) CABG 3) “Bentall” procedure in Acute Aortic dissection. Hemoglobin electrophoresis demonstrated HbS level of more the 40% in all these patients. Before surgery we decided to do perioperative exchange transfusion to
• promote perfusion,
• lower the incidence of perioperative sickling and
• lower the risk of perioperative multi-organ failure.
Hypothermia was prevented by maintaining the perfusate temperature at 35 degrees C. Hypoxia was avoided by maintaining hematocrit values above 24% and by keeping venous saturation above 60%. Frequent monitoring of ABG was done to maintain pH in the normal range. We did a partial exchange transfusion in the operating room for all three patients to reduce the HbS level to less than 20% without any perioperative transfusion. By using a separate reservoir and priming the oxygenator with heterologous blood we were able to reduce the intraoperative circulating HbS level to below 0% after exchange transfusion. This technique, combined with the use of continuous ultrafiltration on CPB, allowed the procedure to be performed without any complications. Cardiopulmonary bypass circuit was primed with 4 units of PRBC. The remaining prime consisted of 2 units of FFP, 100 ml of 20% albumin and sufficient Ringer lactate to complete the total circuit volume of 4 liter. The mixture was pre-oxygenated, warmed and buffered with sodium bicarbonate.
We performed exchange transfusion immediately before the initiation of CPB. After the patient received 3mg/Kg heparin, arterial and venous cannulation was performed. Four liter capacity reservoir was connected with a Y connector to the venous line of the CPB system to enable the perfusionist to collect the patient’s blood before CPB was initiated. Immediately before CPB was started about 3 liters of venous blood, which was estimated to be 2/3 of patient’s blood volume was allowed to rapidly flow in to the reservoir while patient was slowly transfused with 3 liters of solution from CPB system. Once 3 liters of blood was collected in the reservoir, venous flow was redirected to the oxygenator and normal CPB was initiated. Patient’s blood pressure was maintained at 60-70mmHg during exchange transfusion, with the use of vasoactive medications if required.
In the patient with aortic valve replacement and mitral valve repair, we used cold crystalloid cardioplegia. The theoretical advantage of crystalloid cardioplegia over blood cardioplegia is that it would avoid the possibility of sickling and vascular occlusion in coronary microvasculature. Hyperkalemia and hemodilution was avoided by sucking out the crystalloid cardioplegia from the right atrium. During CABG, the heart was initially arrested with 1200 ml of antegrade 4:1 blood–crystalloid cardioplegia maintained at 34 degrees C through the aortic root and in ‘Bentall’ procedure the same combination cardioplegia delivered through coronary ostia. Subsequent doses of cardioplegia at 34 degrees C were given retrograde through coronary sinus at 20-minute intervals. During CPB, flows were maintained at a minimum of 2.4L/m2. Venous saturation was kept above 60% and there was no acidosis during CPB. Arterial pressure was kept between 60 and 90mmHg.
Through pre-operative stabilization of the patient with respect to hemoglobin and use of initial exchange transfusion, customized cardioplegia and maintenance of blood gases, it was possible for CPB to be conducted safely in these sickle cell patients. The successful performance of these cases shows that planning, preparation and cooperation between team members and technical skill can overcome most operative challenges faced by sickle cell patients.